My Waistline
Waist Circumference Measurement Guidelines
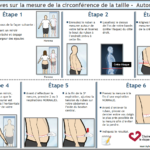
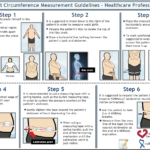
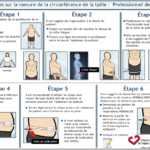
To measure the waist circumference, you can select the self-measurement guidelines or the healthcare professional guidelines below.
More Information about Waist Circumference
Ethnic-specific Waist Circumference
The following table (Table 1) summarizes IDF waist circumference values according to ethnicity and sex. However, these values have not been validated against “hard” clinical outcomes and therefore provide “ballpark” figures to patients and their treating physicians
Clinical Diagnosis
The metabolic syndrome can be diagnosed by primary care physicians (Table 2) and is most often caused by poor eating habits and a sedentary lifestyle that lead to abdominal fat accumulation and insulin resistance (the cells of your body do not respond normally to insulin). You cannot diagnose the metabolic syndrome by yourself. So if you think that your waistline puts you at risk, please see your physician. Prevention is key. Invest in your health!

CMR fun clips
Watch Dr. Cheese and the Potato family’s funny videos and learn simple notions about abdominal obesity and related health.